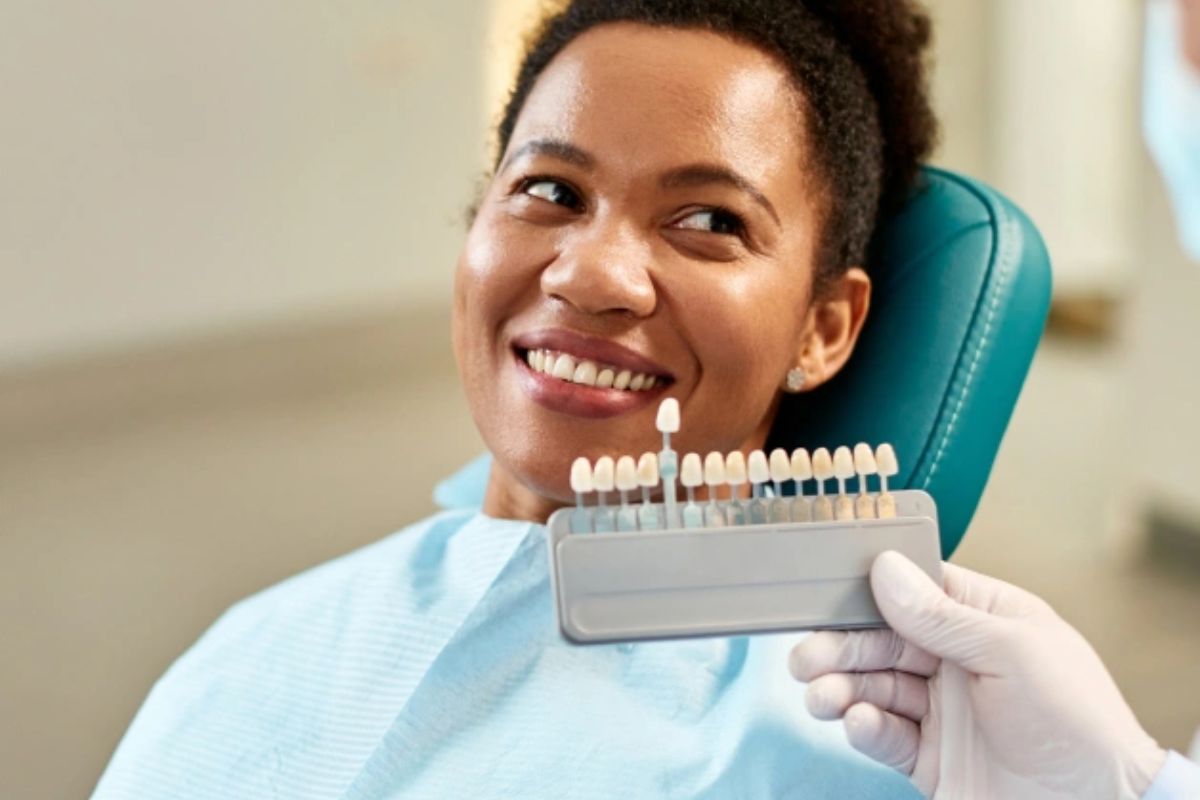
Charcoal toothpaste has become one of the most talked-about oral care products in recent years. From social media influencers to store displays, it is often marketed as a natural solution for achieving a brighter smile. Many people are drawn to the idea of whitening their teeth without undergoing professional treatment. But before adding charcoal toothpaste to your daily routine, it is important to understand what it actually does and whether it lives up to the claims.
Many patients ask about charcoal-based products during dental visits. Some report seeing a temporary improvement in the appearance of their teeth, while others notice increased sensitivity or disappointing results after long-term use. The truth lies somewhere in the middle.
What Does Charcoal Toothpaste Actually Do?
Charcoal toothpaste typically contains activated charcoal, a fine black powder known for its porous structure. This ingredient is believed to absorb and remove certain substances from the surface of the teeth, including stains caused by coffee, tea, red wine, and tobacco.
It can make teeth look slightly cleaner for a short period of time, mostly by polishing away surface buildup. However, it does not change the internal color of your teeth.
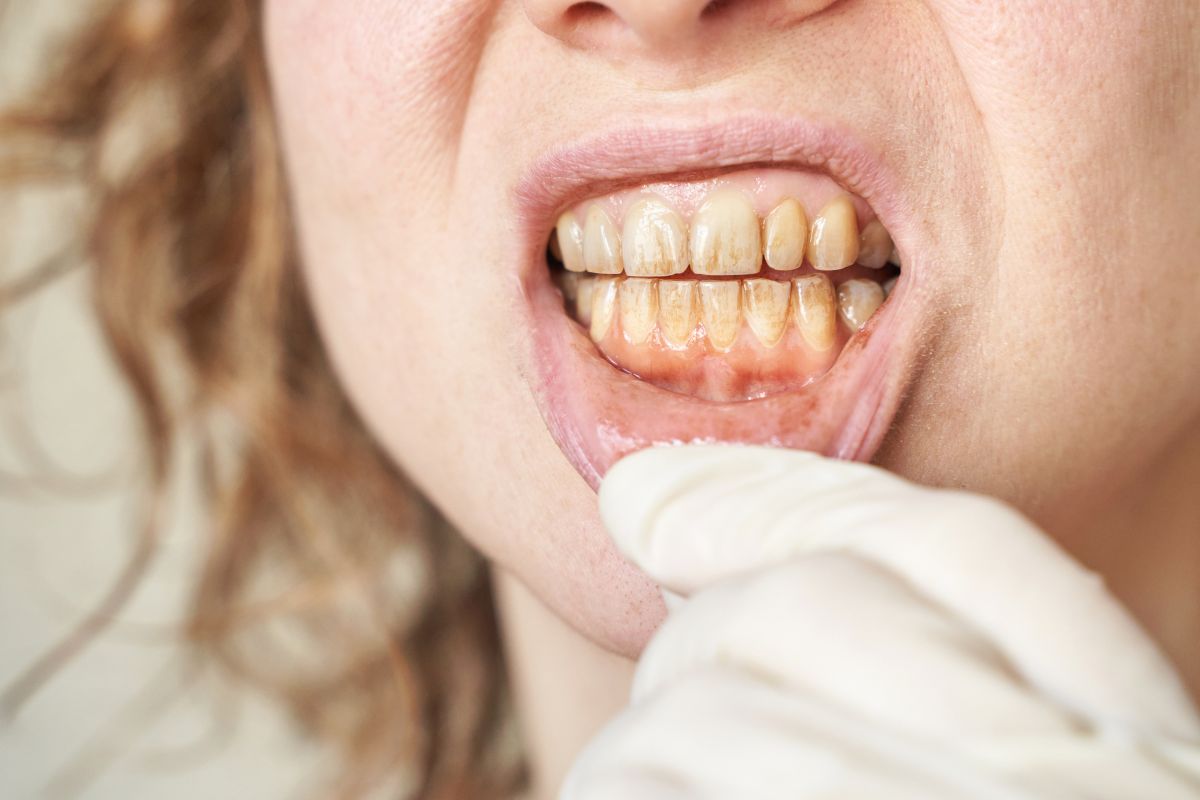
Teeth naturally have layers. The outer layer is enamel, and beneath it lies dentin, which has a slightly yellow tone. As enamel thins over time, the yellow tone becomes more visible. This is where problems can start if abrasive products are used too often.
Charcoal toothpaste does not strengthen enamel or improve long-term brightness. It only works on the surface, which means the results are temporary and limited.
Dentists generally recommend caution with long-term use because enamel protection is more important than short-term brightness.
Does Charcoal Toothpaste Really Whiten Teeth?
The short answer is not what most people expect. Many people associate whitening with dramatically brighter teeth. However, true whitening involves changing the tooth’s internal color, not simply removing surface stains. Since charcoal toothpaste does not penetrate enamel, it cannot effectively address deeper discoloration.
For individuals with mild staining from food and beverages, charcoal toothpaste may provide a temporary cosmetic improvement. However, the results are often subtle and short-lived.
Another important factor is enamel preservation. Some charcoal toothpastes are significantly more abrasive than traditional toothpaste formulations. Over time, repeated abrasion can contribute to enamel erosion, tooth sensitivity, and uneven tooth coloration.
Patients sometimes notice that their teeth initially feel smoother and cleaner after using charcoal toothpaste. Yet after months of use, they may become concerned about increased sensitivity or a duller appearance. This can happen when enamel becomes thinner and less able to reflect light effectively.
Why Everyday Oral Health Still Matters More Than Trends
Teeth whitening is only one part of oral care. The foundation always comes back to daily habits. Brushing twice a day with a fluoride toothpaste, flossing regularly, and keeping up with professional cleanings make a bigger long-term difference than any trending product.
Many patients ask about shortcuts to a brighter smile. The truth is that consistency wins every time. Small daily habits protect enamel and reduce staining naturally.
Even something as simple as drinking water after coffee or rinsing after meals can help maintain a cleaner appearance without risking enamel wear.
Professional Whitening and Why It Works Differently
Professional teeth whitening works very differently from charcoal toothpaste.
Rather than relying on abrasive methods to remove stains, professional whitening treatments use carefully controlled whitening agents that penetrate the enamel and target discoloration beneath the surface. This approach allows for more noticeable, even, and predictable results.
Because the treatment is supervised by dental professionals, the process can be tailored to each patient’s needs. Factors such as enamel thickness, existing restorations, sensitivity levels, and stain severity are all considered before treatment begins.
Professional whitening also includes safeguards that help protect the gums and surrounding tissues. This level of precision is simply not available with over-the-counter whitening products or charcoal-based alternatives.
For patients seeking meaningful improvements in tooth color, professional whitening often provides results that are both more effective and longer lasting.
Bright Smiles Begin with the Right Guidance
It is easy to see why charcoal toothpaste has attracted so much attention. The marketing is appealing, and the idea of a natural whitening solution sounds attractive. However, understanding the limitations of these products can help you make informed decisions about your oral health.
While charcoal toothpaste may remove certain surface stains, it does not offer true whitening and may pose risks when used excessively. Protecting your enamel should always take priority over chasing temporary cosmetic improvements.
If your goal is a brighter smile, a professional evaluation can help determine the safest and most effective option for you. At Syosset Dental, we provide personalized recommendations and professional whitening solutions designed around your individual smile goals. Our team is committed to helping patients achieve brighter, healthier smiles through safe and effective treatment options. Visit our dental office in Syosset and let us help you achieve a healthier, brighter smile with care tailored to your needs.
FAQs About Charcoal Toothpaste for Whitening
1. Does charcoal toothpaste actually whiten teeth?
It can remove some surface stains, which may make teeth look slightly brighter. However, it does not change the internal color of teeth. The effect is usually temporary.
2. Is charcoal toothpaste safe for daily use?
Frequent use may be too abrasive for enamel. Over time, it can contribute to sensitivity and enamel thinning. Dentists usually recommend caution with daily use.
3. Why do my teeth feel different after using charcoal toothpaste?
Charcoal can create a very clean or smooth feeling by polishing the surface. That sensation does not always mean the teeth are healthier or stronger.
4. Can charcoal toothpaste replace professional whitening?
No, it cannot replace professional whitening. Professional treatments target deeper stains and provide more consistent and controlled results.
5. Does charcoal toothpaste work on deep stains?
It mainly affects surface stains only. Deeper discoloration inside the enamel is not treated by charcoal-based products.
6. Can children use charcoal toothpaste safely?
Children should avoid whitening products unless recommended by a dentist. Their focus should be on gentle cleaning and building strong enamel through proper oral care.
7. What is the safest way to get whiter teeth?
The safest approach is a dentist-guided whitening plan combined with good daily oral hygiene. This helps protect enamel while improving overall brightness.